Insulin: A Primer
Insulin is a hormone that regulates the levels of sugar in your blood. When you eat a meal, the carbohydrate in the meal is broken down into glucose (a sugar used as energy by your cells). The glucose enters your blood. Your pancreas senses the rising glucose and releases insulin. Insulin allows the glucose to enter your liver, muscle, and fat cells. Once your blood glucose starts to come back down, insulin levels come back down too. This cycle happens throughout the day. You eat a meal, glucose goes up, insulin goes up, glucose goes down, and insulin goes down. Insulin levels are typically lowest in the early morning since it's usually been at least 8 hours after your last meal.
Insulin doesn't just regulate blood sugar. It has other effects as well. For example, it stimulates your muscles to build new protein (a process called protein synthesis). It also inhibits lipolysis (the breakdown of fat) and stimulates lipogenesis (the creation of fat).
It is the latter effect by which insulin has gotten its bad reputation. Because carbohydrate stimulates your body to release insulin, it has caused some people to argue that a diet high in carbohydrate will cause you to gain fat. Their reasoning, in a nutshell, goes like this:
High Carbohydrate Diet -> High Insulin -> Increased Lipogenesis/Decreased Lipolysis -> Increased Body Fat -> Obesity
Using this same logic, they argue that a low carbohydrate diet is best for fat loss, because insulin levels are kept low. Their logic chain goes something like this:
Low Carbohydrate Diet -> Low Insulin -> Decreased Lipogenesis/Increased Lipolysis -> Decreased Body Fat
However, this logic is based on many myths. Let's look at many of the myths surrounding insulin.
MYTH:A High Carbohydrate Diet Leads to Chronically High Insulin Levels
FACT:Insulin Is Only Elevated During the Time After a Meal In Healthy Individuals
One misconception regarding a high carbohydrate intake is that it will lead to chronically high insulin levels, meaning you will gain fat because lipogenesis will constantly exceed lipolysis (remember that fat gain can only occur if the rate of lipogenesis exceeds the rate of lipolysis). However, in healthy people, insulin only goes up in response to meals. This means that lipogenesis will only exceed lipolysis during the hours after a meal (known as the postprandial period). During times when you are fasting (such as extended times between meals, or when you are asleep), lipolysis will exceed lipogenesis (meaning you are burning fat). Over a 24-hour period, it will all balance out (assuming your are not consuming more calories than you are expending), meaning you do not gain weight. Here's a graph showing how this works:
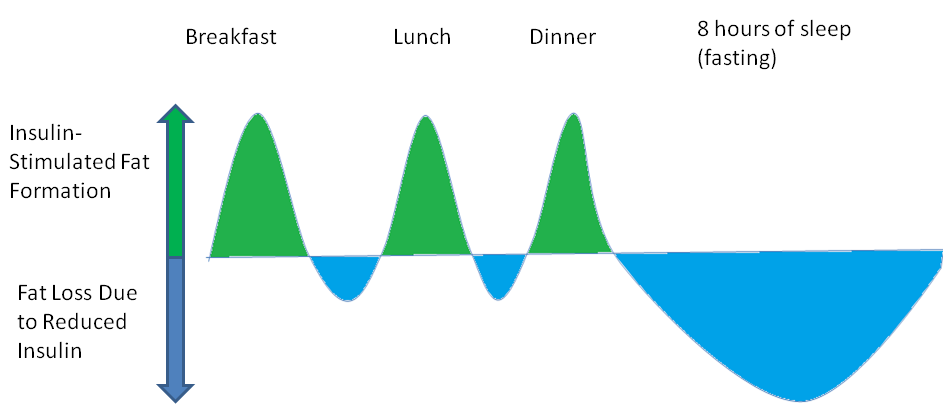
After meals, fat is deposited with the help of insulin. However, between meals and during sleep, fat is lost. Fat balance will be zero over a 24-hour period if energy intake matches energy expenditure.
This is just a rough chart that I made, but the green area represents the lipogenesis occuring in response to a meal. The blue area represents lipolysis occuring in response to fasting between meals and during sleep. Over a 24-hour period, these will be balanced assuming you are not consuming more calories than you expend. This is true even if carbohydrate intake is high. In fact, there are populations that consume high carbohydrate diets and do not have high obesity rates, such as the traditional diet of the Okinawans. Also, if energy intake is lower than energy expenditure, a high carbohydrate diet will result in weight loss just as any other diet.
MYTH: Carbohydrate Drives Insulin, Which Drives Fat Storage
FACT: Your Body Can Synthesize and Store Fat Even When Insulin Is Low
One of the biggest misconceptions regarding insulin is that it's needed for fat storage. It isn't. Your body has ways to store and retain fat even when insulin is low. For example, there is an enzyme in your fat cells called hormone-sensitive lipase (HSL). HSL helps break down fat. Insulin suppresses the activity of HSL, and thus suppresses the breakdown of fat. This has caused people to point fingers at carbohydrate for causing fat gain.
However, fat will also suppress HSL even when insulin levels are low. This means you will be unable to lose fat even when carbohydrate intake is low, if you are overeating on calories. If you ate no carbohydrate but 5,000 calories of fat, you would still be unable to lose fat even though insulin would not be elevated. This would be because the high fat intake would suppress HSL. This also means that, if you're on a low carbohydrate diet, you still need to eat less calories than you expend to lose weight.
Now, some people might say, "Just try and consume 5000 calories of olive oil and see how far you get." Well, 5000 calories of olive oil isn't very palatable so of course I won't get very far. I wouldn't get very far consuming 5,000 calories of pure table sugar either.
MYTH: Insulin Makes You Hungry
FACT: Insulin Suppresses Appetite
It is a well known fact that insulin acutely suppresses appetite. This has been demonstrated in dozens and dozens of experiments. This will be important when we talk about the next misconception...
MYTH: Carbohydrate Is Singularly Responsible for Driving Insulin
FACT: Protein Is a Potent Stimulator of Insulin Too
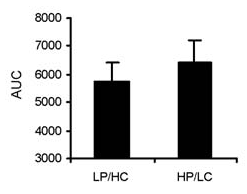
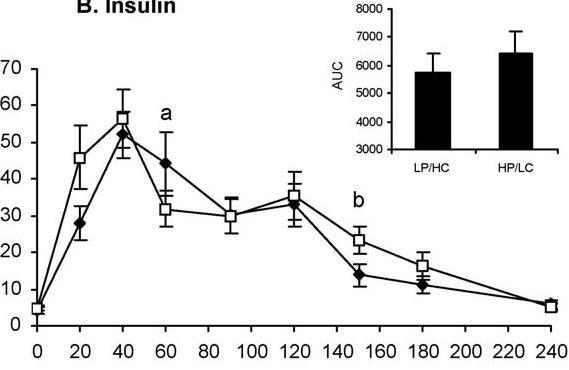
This is probably the biggest misconception that is out there. Carbohydrates get a bad rap because of their effect on insulin, but protein stimulates insulin secretion as well. In fact, it can be just as potent of a stimulus for insulin as carbohydrate. One recent study compared the effects of two different meals on insulin. One meal contained 21 grams of protein and 125 grams of carbohydrate. The other meal contained 75 grams of protein and 75 grams of carbohydrate. Both meals contained 675 calories. Here is a chart of the insulin response:
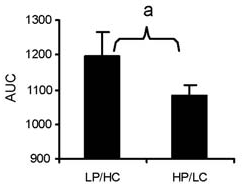
Now here's a chart of the blood sugar response:
You can see that, despite the fact that the blood sugar response was much higher in the meal with more carbohydrate, the insulin response wasn't higher. In fact, the insulin response was somewhat higher after the high protein meal, although this wasn't statistically significant.
Some people might argue that the "low-carb" condition wasn't really low carb because it had 75 grams of carbohydrate. But that's not the point. The point is that the high-carb condition had nearly TWICE as much carbohydrate, along with a HIGHER glucose response, yet insulin secretion was slightly LOWER. The protein was just as powerful at stimulating insulin as the carbohydrate.
I can also hear arguments coming like, "Yeah, but the insulin response is longer and more drawn out with protein." That wasn't true in this study either.
You can see in the chart that there was a trend for insulin to peak faster with the high protein condition, with a mean response of 45 uU/mL at 20 minutes after the meal, versus around 30 uU/mL in the high carb condition.
This tendency for a higher insulin response was associated with a tendency towards more appetite suppression. The subjects had a tendency towards less hunger and more fullness after the high protein meal:

Comparison of low protein, high carb and high protein, low carb meals and their effects on hunger and fullness
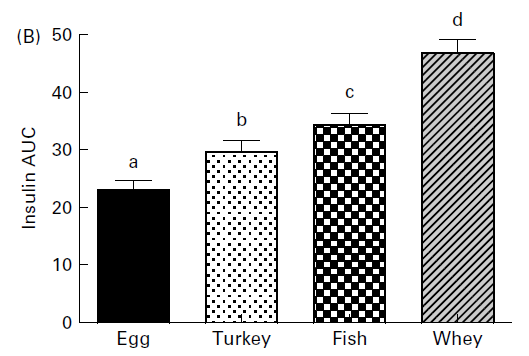
Here's the results of another study that compared the effects of 4 different types of protein on the insulin response to a meal. This study was interesting because they made milkshakes out of the different proteins (tuna shakes???? YUCK!!!!! Of course some people may remember the tuna shake recipes from the misc.fitness.weights days). The shakes contained only 11 grams of carbohydrate, and 51 grams of protein. Here's the insulin response to the different shakes:
You can see that all of these proteins produced an insulin response, despite the fact that the carbohydrate in the shake was low. There was also different insulin responses between the proteins, with whey producing the highest insulin response.
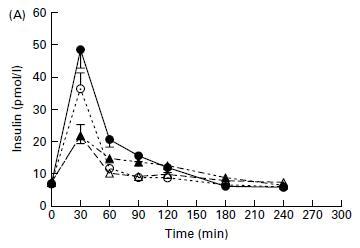
Now, some might argue that the response is due to gluconeogenesis (a process by which your liver converts protein to glucose). The thought is that the protein will be converted to glucose, which will then raise insulin levels. As I mentioned earlier, people will claim that this will result in a much slower, more drawn-out insulin response, since it takes time for your liver to turn protein into glucose. However, that's not the case, because the insulin response was rapid, peaking within 30 minutes and coming back down quickly at 60 minutes:
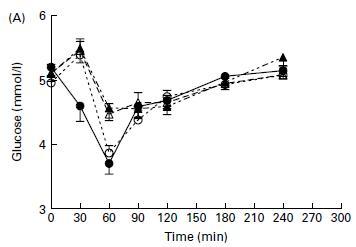
This rapid insulin response was not due to changes in blood glucose. In fact, whey protein, which caused the greatest insulin response, caused a drop in blood glucose:
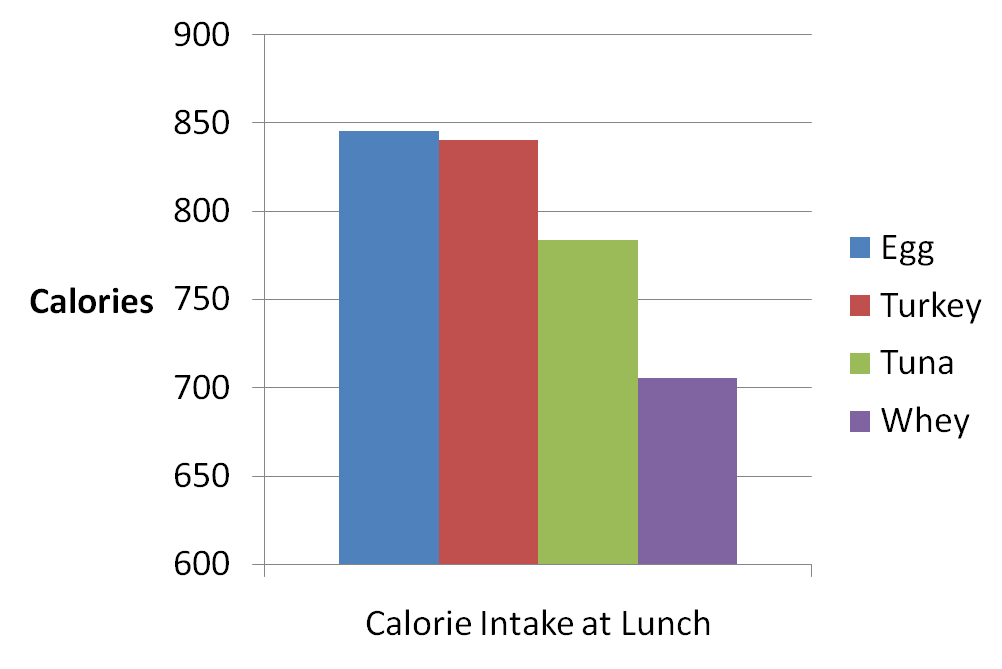
The insulin response was associated with appetite suppression. In fact, the whey protein, which had the highest insulin response, caused the greatest suppression of appetite. Here's a chart showing the calorie intake of the subjects when they ate lunch 4 hours after drinking the shake:
The subjects ate nearly 150 calories less at lunch when they had whey protein, which also caused the greatest insulin response. In fact, there was an extremely strong inverse correlation between insulin and food intake (a correlation of -0.93).
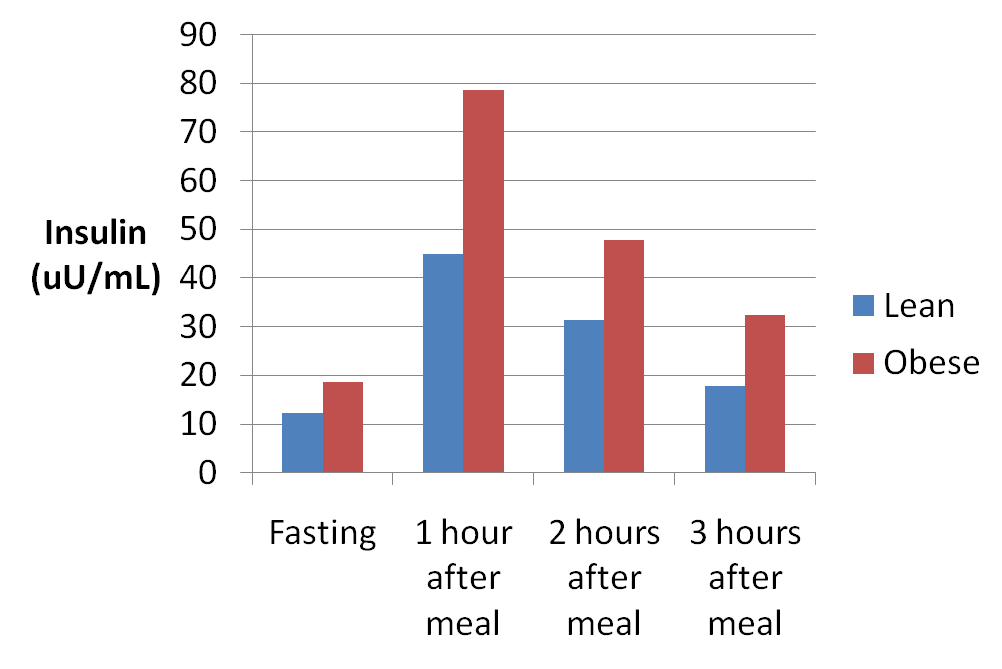
Here's data from another study that looked at the insulin response to a meal that contained 485 calories, 102 grams of protein, 18 grams of carbohydrate, and almost no fat:
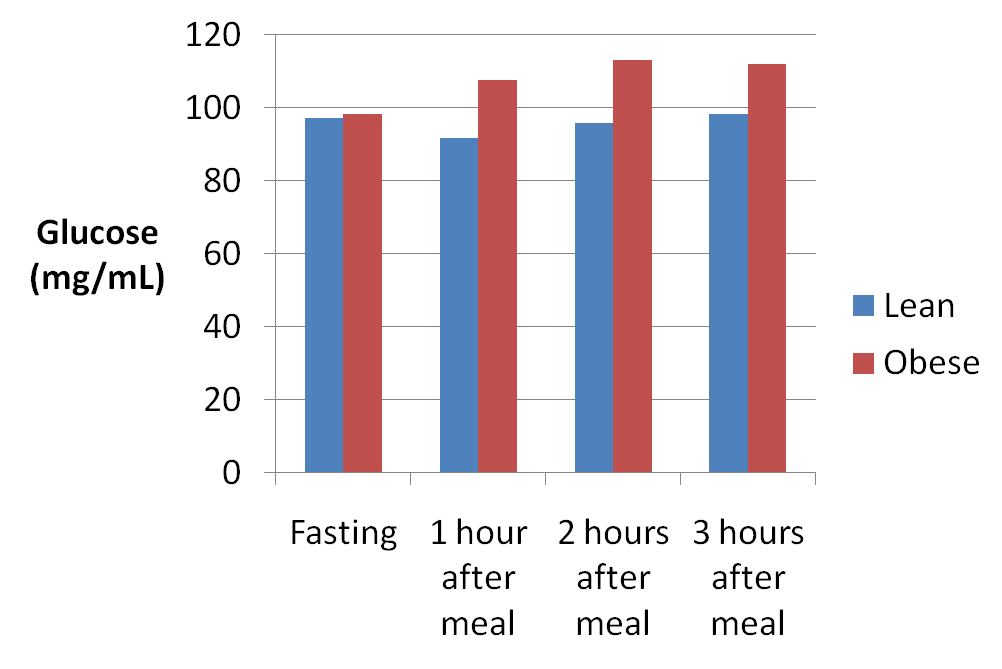
You can see that the insulin response was exaggerated in the obese subjects, probably due to insulin resistance. Here's a chart of the blood glucose response. You can see there was no relationship between the glucose response and insulin, which was similar to the study discussed earlier.
The fact is that protein is a potent stimulator of insulin secretion, and this insulin secretion is not related to changes in blood sugar or gluconeogenesis from the protein. In fact, one study found beef to stimulate just as much insulin secretion as brown rice. The blood sugar response of 38 different foods could only explain 23% of the variability in insulin secretion in this study. Thus, there's a lot more that's behind insulin secretion than just carbohydrate.
So how can protein cause rapid rises in insulin, as shown in the whey protein study earlier? Amino acids (the building blocks of protein) can directly stimulate your pancreas to produce insulin, without having to be converted to glucose first. For example, the amino acid leucine directly stimulates pancreas cells to produce insulin, and there's a direct dose-response relationship (i.e., the more leucine, the more insulin is produced).
Some might say, "Well, sure, protein causes insulin secretion, but this won't suppress fat-burning because it also causes glucagon secretion, which counteracts insulin's effects." I mentioned earlier how insulin will suppress lipolysis. Well, some people think that glucagon increases lipolysis to cancel this out.
The thought that glucagon increases lipolysis is based on 3 things: the fact that human fat tissue has glucagon receptors, the fact that glucagon increases lipolysis in animals, and the fact that glucagon has been shown to increase lipolysis in human fat cells in vitro (in a cell culture). However, what happens in vitro isn't necessarily what happens in vivo (in your body). We have a case here where newer data has overturned old thinking. Research using modern techniques has shown that glucagon does not increase lipolysis in humans. Other research using the same techniques has shown similar results. I will also note that this research failed to find any lipolytic effect in vitro.
It should be remembered why glucagon is released in response to protein in the first place. Since protein stimulates insulin secretion, it would cause a rapid drop in blood glucose if no carbohydrate is consumed with the protein. Glucagon prevents this rapid drop in blood sugar by stimulating the liver to produce glucose.
Insulin: Not Such a Villain After All
The fact is that insulin is not this terrible, fat-producing hormone that must be kept as low as possible. It is an important hormone for appetite and blood sugar regulation. In fact, if you truly wanted to keep insulin as low as possible, then you wouldn't eat a high protein diet...you would eat a low protein, low carbohydrate, high fat diet. However, I don't see anybody recommending that.
I'm sure some are having some cognitive dissonance reading this article right now. I know because I experienced the same disbelief years ago when I first discovered this paper and how protein caused large insulin responses. At the time, I had the same belief that others have...that insulin had to be kept under control and as low as possible, and that spikes in insulin were a bad thing. I had difficulty reconciling that study and my beliefs regarding insulin. However, as time went on, and as I read more research, I learned that my beliefs regarding insulin were simply wrong.
Now, you may be wondering why refined carbohydrates can be a problem. Many people think it's due to the rapid spikes in insulin. However, it's obviously not the insulin, because protein can cause rapid spikes in insulin as well. One problem with refined carbohydrate is a problem of energy density. With refined carbohydrate, it is easier to pack a lot of calories into a small package. Not only that, but foods with high energy density are often not as satiating as foods with low energy density. In fact, when it comes to high-carbohydrate foods, energy density is a strong predictor of a food's ability to create satiety (i.e., low-energy density foods create more satiety). There are other issues with refined carbohydrate as well that are beyond the scope of this article.
The bottom line is that insulin doesn't deserve the bad reputation it's been given. It's one of the main reasons why protein helps reduce hunger. You will get insulin spikes even on a low-carb, high-protein diet. Rather than worrying about insulin, you should worry about whatever diet works the best for you in regards to satiety and sustainability. As mentioned in a previous article, individual responses to particular diets are highly variable and what works for one person will not necessarily work for another. I will be writing a post in the future on the need for individualized approaches to nutrition.
Click here to read part 2 of this series on insulin.

[…] Insulin an undeserved bad reputation (Part I of the series):https://weightology.net/insulin-an-undeserved-bad-reputation/ […]
[…] Insulin an undeserved bad reputation (Part I of the series):https://weightology.net/insulin-an-undeserved-bad-reputation/ […]
so so nice i can only empfählen
[…] lean. Huh? The critics were getting louder, so I read James Krieger’s multi-part series on Insulin: An Undeserved Bad Reputation. It was his analogy that insulin is like a traffic cop that clicked with […]
[…] I am neutral on sugar, I think this fear is likely overstated. Regarding insulin, I suspect Krieger is right, not […]
tHANKS FOR SHARING THIS PERSPECTIVE!
In the article above, you mention: “you would eat a low protein, low carbohydrate, high fat diet. However, I don’t see anybody recommending that.” Isn’t that the KETO Diet? When was this article written?
Keto is typically not low protein
Right, it’s moderate to low protein, doesn’t make much of a difference though.
Thanks a lot, it’s a very significiant article.
With thanks! Valuable information!
That blue/green graph is not accurate in the least. It does not take Glycogen into account. If you’re eating foods which result in insulting spikes, you’re constantly re-filling your Glycogen stores. Thus, in between meals and during sleep you’d be burning STORED CARBS (Glycogen) for the most part, NOT FAT. I feel that Glycogen is forgotten about. Similarly, when people are eating carbs and working out thinking they are burning fat. Well, first you’re burning the carbs, then Glycogen THEN fat. So, why not just cut the carbs, thus depleting the glycogen stores and go straight to burning fat for… Read more »
Yes, the blue/green graph is accurate. First, your body doesn’t switch between burning carbs and fat like some sort of on/off switch. Your body is always oxidizing a mixture of carbs and fat, but the degree for each may vary. It also doesn’t follow the order of “burning carbs, then glycogen, then fat.” It doesn’t work that way…you’re always burning a mix of fuels (and glycogen IS carbohydrate, by the way). Also, you’re wrong about sleep and burning “stored carbs”. At least 50% of resting energy expenditure comes from fat oxidation, regardless of glycogen stores. Whether fat stores are burned… Read more »
No it is accurate, your body stores glycogen in muscles and the liver, however, only the liver glycogen is responsible for balancing out your blood sugar (burned when blood sugar is low). The glycogen in the muscles will not be used, unless if you use the muscle. Even then, you will not burn all the glycogen in your liver all at once. Your liver only stores about 400 cal worth of glycogen, and studies has shown that if you fast, you’ll still have liver glycogen left after 48 hours. On average a person will burn at least 80 cal each… Read more »