In a previous issue of Weightology Weekly, I wrote about insulin and how it's been unfairly demonized by many in the nutrition field. This demonization has been based on a number of misconceptions regarding insulin, its biological effects, and its secretion. I want to continue clarifying these misconceptions.
MYTH: Insulin Spikes are "Bad"
FACT: Insulin Spikes Serve a Normal & Important Physiological Function
In my previous article, I discussed how dietary protein can cause insulin spikes just like dietary carbohydrate, and these spikes are not related to gluconeogenesis from the protein (i.e., the protein being converted to sugar). I also showed how these spikes are partly responsible for the suppression of appetite that is caused by dietary protein (due to insulin's effects on your brain to inhibit appetite).
I want to expand on the importance of rapid insulin spikes due to feeding, and how they are important in blood sugar regulation. To do this, we need to discuss the phases of insulin secretion. Insulin secretion from your pancreas comes in two phases. The first phase happens very quickly; your pancreas senses rising glucose, and insulin is released within 1-2 minutes of this rise in blood sugar. This rapid-phase response is the result of your pancreas releasing stored insulin. It is typically over within 10 minutes. This rapid-phase response has been found to be impaired in people with impaired glucose tolerance (people who have higher blood sugar responses to meals than normal, and higher fasting levels of blood sugar, but who are not diabetic). This rapid-phase response is completely absent in people with type 2 diabetes.
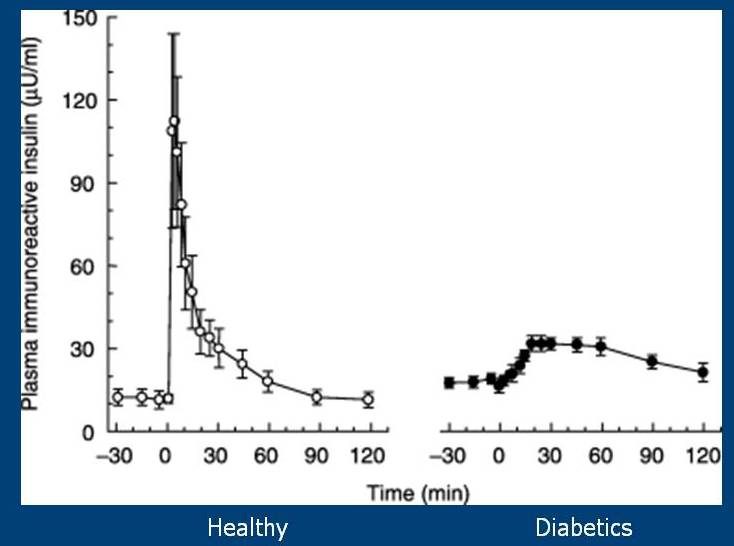
There is a second phase that continues as long as glucose is elevated. This release of insulin is achieved by the release of stored insulin, as well as the creation of new insulin (insulin is created from a precursor called proinsulin). When you infuse glucose into the blood of healthy people and type 2 diabetics, you get insulin responses that look like this:
You can see that the diabetics completely lack the rapid phase response that is present in the healthy individuals.
There is a drug called exenatide (Byetta), which has been found to restore this rapid phase insulin response in diabetics:
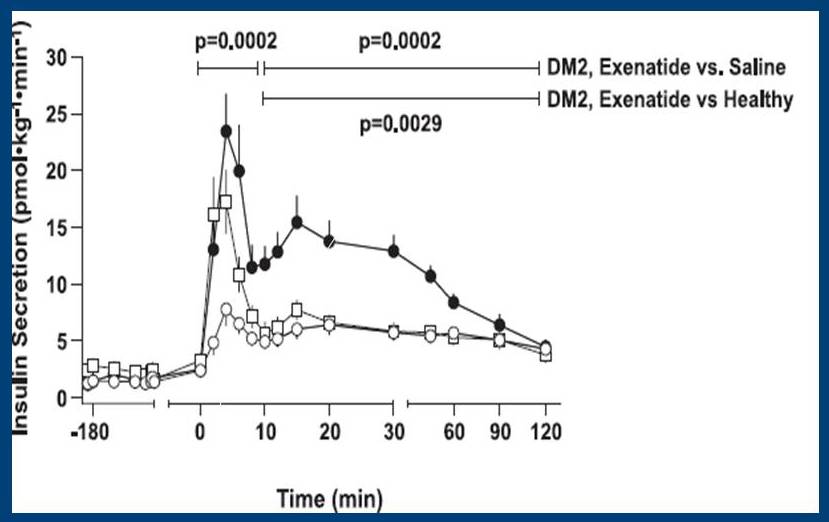
Insulin responses of type2 diabetics and healthy individuals, who have been administered glucose intravenously. Circles represent the insulin response of the type 2 diabetics when given a placebo. Squares represent the insulin response of the diabetics when given exenatide. You can see that exenatide restores the rapid phase insulin response. Black circles represent the insulin response of healthy individuals.
This restoration of the rapid phase insulin response improves blood sugar regulation in diabetics:
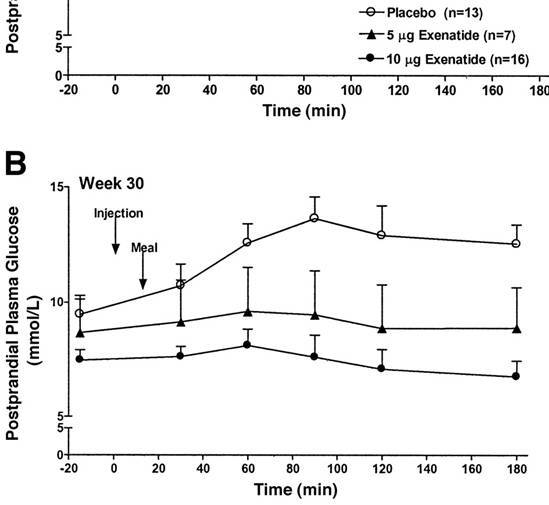
Blood sugar response to a meal in type 2 diabetics. Circles represent subjects on a placebo. Dark triangles and circles represent subjects on exenatide. You can see that blood sugar remained steady in the subjects on exenatide, but gradually increased in the subjects on the placebo.
You can see in the above chart that blood sugar remained consistent in response to a meal in the subjects on exenatide, but it increased over time in the subjects on the placebo.
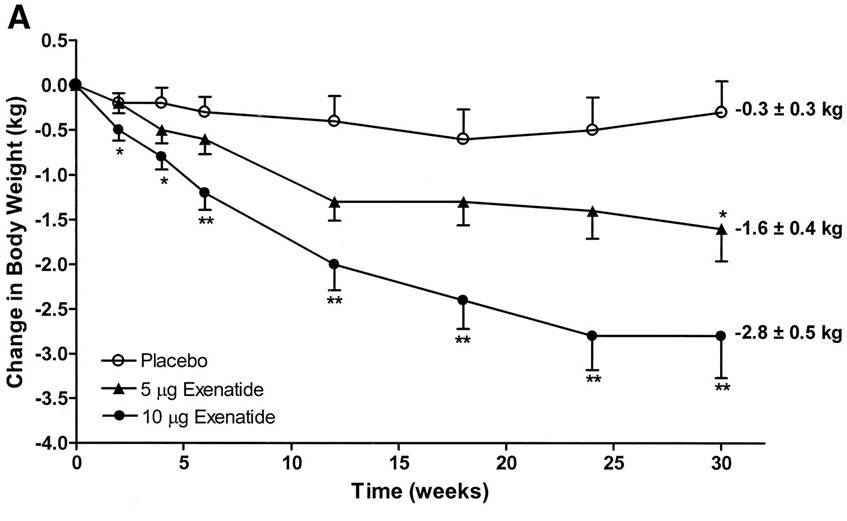
Many people like to blame obesity and weight gain on insulin, but exenatide, which restores insulin spikes in type 2 diabetics, causes weight loss:
Part of this weight loss is due to an improvement in satiety. Exenatide is a drug that mimics the effects of a hormone called glucagon-like peptide-1 (GLP-1). GLP-1 is an intestinal insulin-stimulating hormone (known as an incretin). GLP-1 potentiates insulin secretion, enhances the synthesis of insulin, upregulates insulin gene expression, and inhibits glucagon (insulin's opposing hormone) secretion. Yet Exenatide, which mimics GLP-1 and helps stimulate insulin secretion, causes weight loss.
The fact is that rapid insulin spikes in and of themselves are not a bad thing. Protein causes rapid insulin spikes, yet protein reduces appetite and helps with weight loss. GLP-1 and drugs like exenatide contribute to insulin spikes, yet they reduce appetite and cause weight loss. The problem is that people confuse insulin spikes and blood glucose spikes. It is well established that rapid rises and falls in blood glucose can contribute to hunger. Because rapid rises in blood glucose also cause rapid rises in insulin, people end up blaming insulin (and the effects of high glycemic carbohydrates on insulin) for the problem.
MYTH: Since diabetics who inject insulin gain weight, this means that insulin is the reason for weight gain in non-diabetics
FACT: Amylin is co-secreted with insulin in non-diabetics; amylin has appetite suppressant and lipolytic effects
I would like to thank Dr. Stephan Guyenet for this information. I had known about amylin but hadn't looked into it in any great detail. Amylin is a hormone that is secreted by your pancreas at the same time as insulin. Amylin decreases appetite, and also stimulates lipolysis (the breakdown of fat into fatty acids).
Type 1 diabetics do not produce amylin, and amylin secretion is impaired in type 2 diabetics. Pramlintide, a drug that mimics the effects of amylin, has been found to produce weight loss in diabetics.
This information demonstrates that the effects of insulin injection in a diabetic cannot be compared to the effects of physiological changes in insulin in a non-diabetic, yet many people erroneously make this comparison as if they are similar.
MYTH: Lowering Insulin Will Improve Appetite Regulation
FACT: Insulin Is One of the Many Hormones Critical to Satiety
I already most addressed this myth in my previous article on insulin, showing how protein stimulated insulin secretion and helped reduce appetite, and also showing how insulin injection into the brain reduces appetite. I again want to thank Dr. Guyenet for this information, but when you knock out the insulin receptors of a mouse's brain, the mouse will overeat and develop obesity.
MYTH: All of this information only applies to healthy people
FACT: The information applies to obesity and diabetes
On other forums, I saw people comment on my previous article and claim that the information I provided only applied to healthy people, and not diabetics or obese individuals. They continued to believe that treating diabetes and obese individuals was all about insulin control. Nothing could be further from the truth. Not only is this evident from information mentioned earlier in this article (such as how exenatide restores insulin spikes and improves blood sugar control and body weight in diabetics), but it is also evident from the fact that high protein diets have been found to help both diabetics and obese individuals, despite the fact that protein is a powerful stimulus of insulin secretion.
As I mentioned earlier, people seem to confuse blood glucose control and insulin control. It is the management of blood glucose itself that is partly responsible for the health benefits of low-glycemic carbohydrates, or reducing carbohydrates, or increasing protein intake, or consuming dietary fiber, or consuming fruits and vegetables, or consuming whole foods over processed foods. It is not the control of insulin; the control of insulin ends up being a byproduct of these other behaviors through improvements in insulin sensitivity (how responsive your cells are to insulin) and reductions in blood sugar swings.
Remember, insulin is not the bad guy. Click here to read part 3 of this series, where I discuss how dairy products are extremely insulinemic, yet do not promote weight gain.

It’s hard to argue with the studies sited in this article and the previous article. And you can’t doubt the underlying physiology and biochemistry in play here. You also can’t deny the fact that insulin will allow the storage of CHO as fat if eaten in excess to the dose response capacity. Also that in the presence of insulin fat cells do not release FA and they are more receptive to uptake of glucose. Basically it is not necessary to “de-villainize” insulin. Insulin does not cause weight gain and many of the Low carb proponents may say that to simplify… Read more »
Finally someone’s saying the right thing – sugar is the reason. Insulin is a mechanism. If not insulin, something else would be the mechanism. And in the absence of this mechanism we would not live. Insulin is the life saver – its helping you clear the sugar from the bloodstream – if not for this ‘good guy insulin’ we would not live. Insulin is NOT making you fat. Sugar – is making you fat. To fix the problem you would eliminate the source (Sugar). Not the saving mechanism (Insulin). Its responding to the threat of Sugar every time – like… Read more »